Health
Doctors Urge Action as Cervical Cancer Rates Soar in Canada
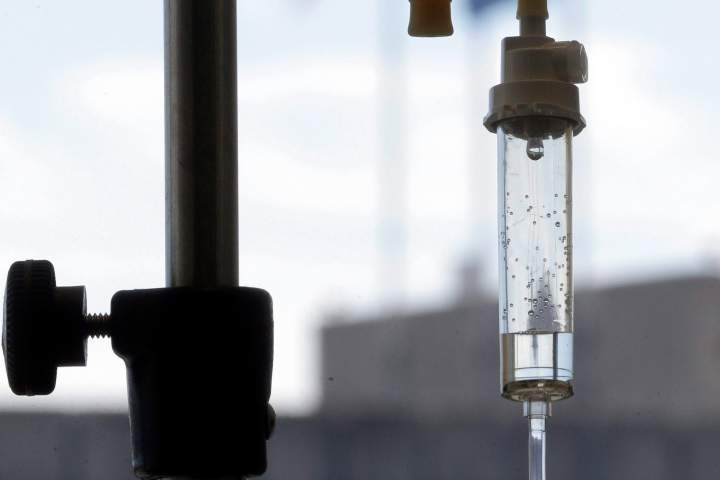
Cervical cancer has emerged as the “fastest-rising form of cancer” in Canada, prompting urgent calls from medical professionals for increased federal action. During a press conference held on Wednesday in Ottawa, members of the Society of Gynecologic Oncology of Canada emphasized that the issue represents a “silent national health crisis.” This statement follows the Canadian government’s action plan, released in July 2025, which aims to “eliminate cervical cancer as a public health problem by 2040.”
Dr. Shannon Salvador, president of the Society of Gynecologic Oncology of Canada, highlighted alarming statistics during the press conference. In 2025, an estimated 1,650 Canadians were diagnosed with cervical cancer, with 430 fatalities projected as a result of the disease, which she described as “avoidable.” The reliance on Pap testing and insufficient levels of human papillomavirus (HPV) vaccination were identified as critical factors contributing to this rise.
Salvador pointed out that Canada’s strategy has not kept pace with advancements in medical science. “For years, we have relied on Pap testing, and our initial enthusiasm for the HPV vaccine upon its first debut in the mid-2000s has not translated into effective policy,” she stated. Current national HPV vaccination rates are stagnant at 64 percent, significantly below the target necessary for effective elimination of cervical cancer.
The Society is advocating for an “immediate, national shift in HPV DNA testing for cervical cancer screening” and the implementation of “HPV self-collection swabs and kits.” These kits would allow individuals to perform at-home tests, addressing barriers related to travel, past trauma, cultural marginalization, and the lack of accessible healthcare providers. Salvador emphasized that this approach is particularly vital for people in rural, Indigenous, and underserved communities who often face systemic healthcare challenges.
Dr. Sarah Kean, provincial lead for cervical cancer in Manitoba, further elaborated on the disparities faced by Indigenous women. She noted that they are diagnosed at higher rates with more advanced stages of the disease, resulting in poorer health outcomes. “This is not due to biology,” Kean explained, “but rather barriers such as geographic isolation, systemic racism in healthcare, and the ongoing impacts of colonial practices.” She called for a “robust, accessible HPV screening” initiative across Canada, which must include universal access to primary HPV testing with clear national standards.
In a related context, reality television star Nicole “Snooki” Polizzi recently announced her diagnosis of Stage 1 cervical cancer, detected through a cone biopsy. This highlights the importance of early detection, as Salvador noted that the financial burden of treating cervical cancer on the Canadian healthcare system was approximately $132 million in 2024. The cost of screening eligible Canadians over the next five years is expected to total $106 million.
A report released by the Canadian Cancer Society (CCS) in November 2025 indicated that progress in combating cervical cancer has stagnated despite global efforts. According to the report, cervical cancer is currently the “fourth most diagnosed cancer and fourth leading cause of cancer death among females worldwide.” In Canada, it was projected that 1,600 females would be diagnosed in 2024, with 400 deaths resulting from the disease.
Historically, cervical cancer rates had been declining between 1984 and 2005, with an annual decrease of 2.2 percent. However, the period from 2005 to 2021 saw a marked slowdown, with only a 0.3 percent annual decrease on average. Kean underscored the importance of the commitments made by both Canada and the World Health Organization (WHO) to eliminate cervical cancer, which hinge on three critical components: vaccination, HPV-based DNA screening, and access to treatment.
“Cervical cancer is one of the most preventable cancers,” Kean concluded. “All other cancers in our country are decreasing in incidence except for the one that is entirely preventable.” The call to action from health professionals underscores the urgent need for comprehensive strategies that address both prevention and equitable access to care in order to effectively tackle this growing health crisis.
-

 Education7 months ago
Education7 months agoBrandon University’s Failed $5 Million Project Sparks Oversight Review
-

 Science7 months ago
Science7 months agoMicrosoft Confirms U.S. Law Overrules Canadian Data Sovereignty
-

 Lifestyle7 months ago
Lifestyle7 months agoWinnipeg Celebrates Culinary Creativity During Le Burger Week 2025
-

 Education7 months ago
Education7 months agoNew SĆIȺNEW̱ SṮEȽIṮḴEȽ Elementary Opens in Langford for 2025/2026 Year
-

 Business4 months ago
Business4 months agoEngineAI Unveils T800 Humanoid Robot, Setting New Industry Standards
-

 Health7 months ago
Health7 months agoMontreal’s Groupe Marcelle Leads Canadian Cosmetic Industry Growth
-

 Science7 months ago
Science7 months agoTech Innovator Amandipp Singh Transforms Hiring for Disabled
-

 Lifestyle3 months ago
Lifestyle3 months agoDiscover Aritzia’s Latest Fashion Trends: A Comprehensive Review
-

 Technology7 months ago
Technology7 months agoDragon Ball: Sparking! Zero Launching on Switch and Switch 2 This November
-
 Technology2 months ago
Technology2 months agoDigg Relaunches as Founders Kevin Rose and Alexis Ohanian Join Forces
-

 Top Stories3 months ago
Top Stories3 months agoCanadiens Eye Elias Pettersson: What It Would Cost to Acquire Him
-

 Health6 months ago
Health6 months agoEganville Leader to Close in 2026 After 123 Years of Reporting
-

 Education7 months ago
Education7 months agoRed River College Launches New Programs to Address Industry Needs
-

 Business6 months ago
Business6 months agoRocket Lab Reports Strong Q2 2025 Revenue Growth and Future Plans
-

 Top Stories3 months ago
Top Stories3 months agoNicol Brothers Shine as Wheat Kings Dominate U18 AAA Hockey
-

 Business7 months ago
Business7 months agoBNA Brewing to Open New Bowling Alley in Downtown Penticton
-

 Education5 months ago
Education5 months agoAlberta Petition Aims to Redirect Funds from Private to Public Schools
-

 Technology7 months ago
Technology7 months agoGoogle Pixel 10 Pro Fold Specs Unveiled Ahead of Launch
-

 Technology6 months ago
Technology6 months agoDiscord Faces Serious Security Breach Affecting Millions
-

 Education7 months ago
Education7 months agoAlberta Teachers’ Strike: Potential Impacts on Students and Families
-

 Lifestyle2 weeks ago
Lifestyle2 weeks agoCanmore’s Le Fournil Bakery to Close After 14 Successful Years
-

 Business7 months ago
Business7 months agoIconic Golden Lion Restaurant in South Surrey to Close After 50 Years
-

 Science7 months ago
Science7 months agoChina’s Wukong Spacesuit Sets New Standard for AI in Space
-

 Lifestyle5 months ago
Lifestyle5 months agoEdmonton’s Beloved Evolution Wonderlounge Closes, New Era Begins